Greta Kaplan, CPDT Recently, I engaged in a discussion with a poster to a dog training list. The poster is a breeder of an AKC toy breed, and she had two intact, year-old males who were fighting. It sounded like one was resource guarding her and the other, she mentioned, was very shy. In responding,… [Read More]
Dog Training & Behavior

Cat behavior and misbehavior
By peggy 10 Comments
Jim Ha, PhD, CAAB Cats are a mystery to many of their owners, perhaps more so than dogs. Dogs are social, like we primates, and so we can often understand their need for attention, the reward of social contact and praise, and even, at a deeper evolutionary level, perhaps a lot of their signals and… [Read More]

Canine assistants for dog/dog fear & aggression
By peggy 3 Comments
Greta Kaplan, CPDT One of the most difficult practical aspects of working with reactive or aggressive dogs is creating practice scenarios where the client’s dog can be exposed to his triggers in a controlled fashion. Owners often assume we can meet at the dog park, because that is where the dog is having the problem…. [Read More]

Chicken Camp, Part 1
Greta Kaplan, CPDT Of all the education I’ve experienced in becoming and being a dog trainer, the one that stands out most is what’s known as “Chicken Camp.” More properly called “Cross-Species Operant Conditioning Training Workshop” (you can see why people prefer to call it Chicken Camp), this workshop teaches advanced, high-quality clicker training skills… [Read More]
Cat Behavior & Training

Cat behavior and misbehavior
By peggy 10 Comments
Jim Ha, PhD, CAAB Cats are a mystery to many of their owners, perhaps more so than dogs. Dogs are social, like we primates, and so we can often understand their need for attention, the reward of social contact and praise, and even, at a deeper evolutionary level, perhaps a lot of their signals and… [Read More]

Tips For Getting Your Cat To The Veterinarian
By peggy 5 Comments
Miles Bensky, BA, CTC When I read the September edition of the Animal Behavior Associates newsletter, I found a statistic that was quite alarming. It was estimated that 36% of the 81 million cats in the United States did not see a vet in 2006. Why are so many cats not receiving regular healthcare? Regular… [Read More]

Kitten Socialization
By peggy 6 Comments
Jim Ha, PhD, CAAB Cats, like all mammals, are social creatures. While cats are far less social than dogs, to think of cats as asocial is wrong. The degree of social behavior and the ability of an individual to adapt to a changing social environment varies with species (certainly cats are less social than dogs),… [Read More]

I Have Four Cats, One Dog, and Two Pet Peeves
Louisa Beal, DVM I like to consider myself a fairly non-judgmental person. People may do things to their pets that I think are horrible, but I cannot judge them, since, in the past, I have done most of those things myself. We all grow and learn and change. However, there are two things that get… [Read More]
Pet Health
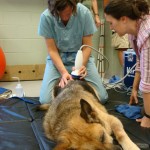
Rehabilitation Therapy for Dogs
[By peggy 6 Comments
Christine Hibbard, CTC, CPDT-KA Many of the medical treatments that have been available to human patients are more commonly becoming available for our pets. In fact, some research being done at veterinary schools like Purdue and research centers in veterinary oncology are furthering human research and treatments. When I got curious about water therapy and… [Read More]

Do You Dread Going to the Veterinarian?
[By peggy 7 Comments
Christine Hibbard, CPDT-KA and Anna Baxter, LVT Do you dread trips to the veterinarian with your dog or cat? Do you wonder if the veterinarians and vet techs dread your visit as much as you do? The veterinary staff needs to be able to perform thorough examinations, provide treatments and perform procedures. How can they… [Read More]

Western Veterinary Conference 2011
[By peggy Leave a Comment
Guest Blogger: Anna Baxter, BA, LVT Recently I attended the Western Veterinary Conference, one of the largest gatherings of veterinary practitioners in the world, for some continuing education. My focus was Behavior, where I went to all 20 hours of scientific programming by some of the best in the industry. Some of the speakers (DVMs)… [Read More]

Don’t Touch Me There!
[By peggy 2 Comments
Louisa Beal, DVM Mario, a West Highland White Terrier had snapped at a two year old girl. If Mario couldn’t be trusted around children, his owners would have to get rid of him. The knee jerk response to this would be to try to modify the behavior of the dog. Mario’s behavior is definitely unacceptable. … [Read More]
